Man refused liver for using medical marijuana
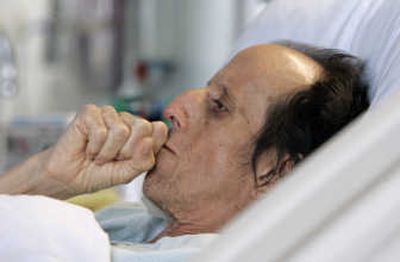
SEATTLE – Timothy Garon’s face and arms are hauntingly skeletal, but the fluid building up in his abdomen makes the 56-year-old musician look 8 months pregnant.
His liver, ravaged by hepatitis C, is failing. Without a new one, his doctors tell him, he will be dead in days.
But Garon isn’t getting a new liver. He’s been refused a spot on the transplant list, largely because he has used marijuana, even though it was legally approved for medical reasons.
“He said I’m going to die with such conviction,” said Garon, lying in his hospital bed a few minutes after a doctor told him the hospital transplant committee’s decision Thursday. “I’m not angry. I’m not mad. I’m just confused.”
Because of the scarcity of donated organs, transplant committees like the one at the University of Washington Medical Center have tough standards for deciding who should get them. Does a candidate have other serious health problems? Will he religiously take anti-rejection medicines? Is there good family support? Is the candidate likely to drink or do drugs?
Garon believes he got hepatitis by sharing needles with “speed freaks” as a teenager. In recent years, he says, pot has been the only drug he’s used. In December, he was arrested for growing marijuana.
His case poses a new ethical consideration for those allocating organs, one that could become more common as a dozen states now have medical marijuana laws: When dying patients need a transplant, should it be held against them if they’ve used dope with a doctor’s blessing?
“Most transplant centers struggle with issues of how to deal with people who are known to use marijuana, whether or not it’s with a doctor’s prescription,” said Dr. Robert Sade, director of the Institute of Human Values in Health Care at the Medical University of South Carolina. “Marijuana, unlike alcohol, has no direct effect on the liver. It is, however, a concern … in that it’s a potential indicator of an addictive personality.”
The Virginia-based United Network for Organ Sharing, which oversees the nation’s transplant system, leaves it to individual hospitals to develop criteria for transplant candidates. At some, people who use “illicit substances” – including medical marijuana, even in states that allow it – are automatically rejected. At others, such as the UCLA Medical Center, patients are given a chance to re-apply if they stay clean for six months. Marijuana is illegal under federal law.
Garon, who has been hospitalized or in hospice care for two months straight, said he turned to the university hospital after Seattle’s Harborview Medical Center told him he needed six months of abstinence. The university also denied him but said it would reconsider if he enrolled in a 60-day drug-treatment program.
This week, at the urging of Garon’s lawyer, Douglas Hiatt, the university’s transplant team reconsidered anyway, but it stuck to its decision.
Dr. Brad Roter, the Seattle physician who authorized Garon’s pot use for nausea, abdominal pain and to stimulate his appetite, said he did not know it would be such a hurdle if Garon were to need a transplant. That’s typically the case, according to Peggy Stewart, a clinical social worker on the liver transplant team at UCLA who has researched the issue.
“There needs to be some kind of national eligibility criteria so that everyone will know what the rules are,” Stewart said. The patients “are trusting their physician to do the right thing. The physician prescribes marijuana, they take the marijuana, and they are shocked that this is now the end result.”
No one tracks how many patients are denied transplants over medical marijuana use. Pro-marijuana groups have cited a handful of cases, including at least two patient deaths, in Oregon and California, since the mid-to-late 1990s, when states began adopting medical marijuana laws.
Another Seattle-area patient, Jonathan Simchen, 33, of Fife, said he was rejected as a kidney-transplant candidate at Virginia Mason Hospital and told by UW that he will not be listed until he abstains from pot for six months. Simchen said he uses marijuana to control his blood pressure and to stimulate his appetite, which is disrupted by dialysis.
Many doctors agree that using marijuana – smoking it, especially – is out of the question post-transplant. The drugs patients take to help their bodies accept a new organ increase the risk of aspergillosis, a frequently fatal infection caused by a common mold found in marijuana and tobacco.
But there’s little information on whether using marijuana is a problem before the transplant, said Dr. Emily Blumberg, an infectious disease specialist who works with transplant patients at the University of Pennsylvania Hospital.
Further complicating matters, Blumberg said, is that some insurers require proof of abstinence, such as drug tests, before they’ll agree to pay for transplants.
“You look at each person and determine what the significance is of whatever they’re taking, and if there’s a potential inappropriate use,” she said.