Patients find disadvantage to private Medicare plans
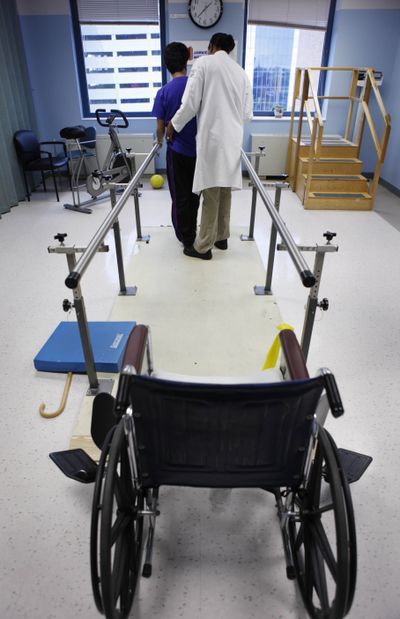
MIAMI – Cecile Sangiamo liked her health insurance – until she needed to use it.
The 72-year-old Clearwater, Fla., resident had been on the federally subsidized, privately run Medicare Advantage policy through WellCare Inc. for about three years when she started having pain that made it hard to walk.
Her doctor’s referral to an orthopedic specialist was denied by the insurer. Her out-of-pocket costs were higher than she was initially told. And when Sangiamo needed surgery, she said, WellCare offered some unexpected medical advice.
“Take pills and use a walker,” Sangiamo remembered being told by the insurer, which declined to comment on the case. “I wanted to say, ‘I’ll take the walker and bang you in the head with it.’ ”
Seniors have flocked by the millions to Medicare Advantage, privately run plans offered as an alternative to traditional, government-run Medicare. Programs that promise lower premiums or other perks have combined with heavy marketing from insurance companies to make the programs double in size in the past six years to nearly 11 million members and growing.
But critics say the plans put profits above care and denials of service are routine.
Profits at the insurers offering Medicare Advantage have far outpaced expectations, and their expenses to treat clients have been far lower than projected.
Advantage insurers are required to offer perks beyond traditional Medicare, such as gym memberships or hearing aids. Enrollees also often get care coordination among the many doctors an older person might have. But there is no standardization of the thousands of plans seniors can choose from, and co-pays and premiums vary widely.
In the debate on overhauling the U.S. health care system, Advantage has been criticized as an example of a broken system that costs too much, confuses enrollees and suffers from a lack of oversight.
Government payouts for Advantage of $111 billion a year and, on average, 14 percent more per patient than traditional Medicare have made the plans a key target for lawmakers and President Barack Obama, who has cited it frequently as too costly.
Proponents of Advantage and the many seniors who like their coverage hail its added benefits and care coordination. But even many backers acknowledge one of its toughest problems is few seniors understand the essential difference in private plans: Even services covered by traditional Medicare that doctors deem medically necessary routinely need the insurers’ advance approval and are sometimes denied.
“There are so many hoops to run through, there are so many rules, it’s just mind-boggling,” said Mary Johnson, policy analyst for the Senior Citizens League, a nonpartisan, 1.2 million-member group.
Participants have been denied visits to specialists, rehabilitation to help them walk again and countless other services they’d be entitled to under traditional Medicare.
“Every decision is based on not what’s right for the patient, but what’s right for the bottom line,” said Dr. Michael Sedrish, who coordinates HMO payments for Medisys Health Network, which runs three New York City hospitals.
Subsidies boosted enrollment
Everyone over 65 and many disabled people qualify for Medicare. Private plans, paid for by the government but run by private insurers, were added in the 1970s to give added choices in coverage.
In 2003, the government added lucrative subsidies for insurers, now totaling more than $15 billion a year. Many more companies got into the business, with massive marketing efforts, and enrollment went from 5.3 million in 2003 to more than 10.7 million in July.
With basic Medicare, seniors generally know what sort of coverage they’re getting. That’s not the case with the roughly 7,000 Medicare Advantage plans, where one person’s coverage could be completely different from a next-door neighbor’s.
Another notable difference between traditional Medicare and Advantage plans is that the vast majority of traditional Medicare denials come after treatment, when the doctor or hospital is fighting to get paid.
Wide differences in enrollee costs
Enrollees in both traditional and private plans pay part of the costs. Under traditional Medicare, many carry an additional private policy, known as MediGap, to cover what the government doesn’t, and that policy can cost a few hundred dollars per month.
Seniors often join Advantage plans because they think they’ll cut expenses through lower premiums or co-pays, and this can be true. But it’s difficult to tell when signing up, because the benefit rules can be daunting and medical issues can crop up unexpectedly.
A 2008 Government Accountability Office report found wide differences in enrollee costs depending on the plan, including home health service costs that could be up to 84 percent more than traditional Medicare.
A half-million Advantage enrollees were in plans with no co-pay for hospital stays. But a roughly equal number were in plans with high hospital co-pays and no limits on out-of-pocket inpatient expenses, potentially costing patients thousands more.
The disparity was greatest for some of the sickest seniors, the GAO found – those who return to the hospital within 60 days of discharge. Under traditional Medicare, those patients would not pay any deductible. Under many Advantage plans, it could be steep.
“The plans tell them they have the same coverage,” said Delores Bowman, who handles calls to the Medicare Rights Center, “and they don’t.”
The independent nonprofit helps Medicare enrollees, and the makeup of its roughly 10,000 annual calls has changed dramatically, dominated by complaints from Medicare Advantage customers.
“The HMOs seem to deny everything,” she said.
Dealing with denial
At Jamaica Hospital in New York, it all became clear with Angela Dispenza.
The New Yorker was a healthy 77-year-old when she fell two years ago and fractured her back.
Doctors thought it obvious that Dispenza should be admitted to the hospital, then receive rehabilitation as her best chance to walk again. The hospital says her Medicare Advantage plan, Oxford, denied her hospital admission, rehabilitation and even an ambulance ride home.
The hospital admitted Dispenza anyway. It was paid, though not in full, only after going public with the case. Dispenza was able to walk out of the hospital on her own; doctors said she would have been bedridden and died without the treatment they insisted on.
Sedrish, whose Medisys network of hospitals in New York owns Jamaica Hospital, found her case such an egregious example of denials he says he sees so often that he set out to prove it.
He analyzed files for 16 months in 2006 and 2007, looking only at patients from on insurer, Oxford, in need of just two types of care, acute rehabilitation and treatment for traumatic brain injuries. Of 46 such cases, the hospital says, all but three were denied.
Oxford declined to comment.
“There are barriers on top of barriers on top of barriers to try and prevent people to get the services,” Sedrish said. “No one ever gave these insurance companies the right to decide who should live and who should die.”