Bringing lives into focus
Improved technology makes Lasik surgery less risky for patients, doctors
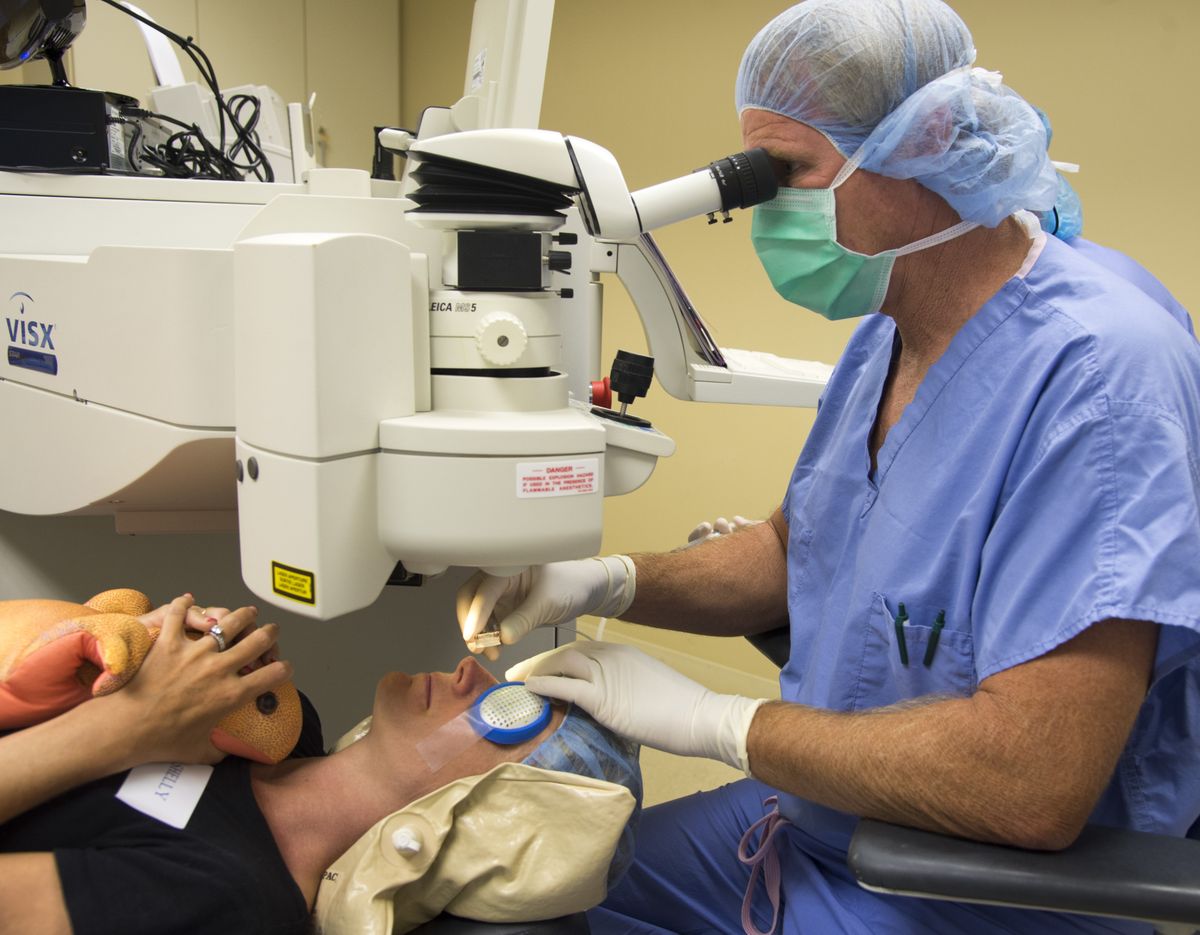
Her right eye forced wide open with a metal speculum, Shelly Buckholz sat still in her chair, hands folded over the orange stuffed reptile provided by a technician as a laser emitted pulses of energy into her eye – essentially cutting a flap in her cornea.
Buckholz’s surgeon used a thin, wet sponge to push the flap aside so he could use more laser energy to reshape an inner layer of her cornea, changing her eye’s ability to focus and improving her vision.
While Buckholz was nervous before her 10-minute Lasik surgery – “I’m glad I took a Valium,” she said – the 44-year-old’s faulty eye was No. 20,000 or so for the surgeon, Dr. Mark Kontos, of Empire Eye Physicians in Spokane.
Surgeons have been performing Lasik surgery to improve patients’ vision for 15 years with approval from the U.S. Food and Drug Administration, and some a few years longer than that, making off-label use of tools approved for other procedures before Lasik got the green light in 1998.
The vast majority of patients have praised their results – clear vision for little discomfort – but some have lodged complaints with the FDA about the surgery’s side effects, including dry eye, glare and double vision. The agency is in the midst of a multipart study launched in 2009 to learn more about the surgery’s long-term effects.
Before the results are tallied – and it might be awhile, as participants are still being recruited – eye doctors who perform the surgery say Lasik technology has evolved since surgeons first offered the procedure, reducing risk. And many surgeons have gotten better at turning away patients who are poor Lasik candidates, citing industrywide experience and technology that provides more detailed information about the structure of patients’ eyes.
“We just know a lot more than we used to know,” said Kontos, Buckholz’s surgeon, who started performing Lasik surgery in 1996.
Buckholz, who lives in Liberty Lake, said she was warned of possible side effects and risks, including blurriness, itchiness and a “halo effect” in her vision. A scary one, she said, was the risk “that you can’t see.”
But the risks were described to her as minimal – in her mind, worth the chance to improve her vision and shed her glasses.
Still, there’s room for caution for patients considering Lasik, doctors say.
“We tell everybody that even though it’s lasers and even though it’s been proven to be safe and it’s effective, there’s still a risk, and they have to be willing to take that small risk,” said Dr. James Salz, a spokesman for the American Academy of Ophthalmology and a clinical professor of ophthalmology at the University of Southern California.
Reshaping corneas
Lasik surgery, or “laser-assisted in situ keratomileusis,” works by changing the shape of the cornea, changing the eye’s ability to focus. It’s used to treat nearsightedness, farsightedness and astigmatism, which can blur or distort how patients see objects both near and far.
Doctors use a blade or a laser to cut a flap in the cornea, the clear part of the front of the eyeball that covers the iris and pupil and lets light inside. The flap is folded back to reveal the cornea’s middle section, called the stroma. A laser is used to remove part of the stroma, and the flap is put back in place to heal.
Whether the doctor uses a blade or a laser is important, Salz said. The biggest change in Lasik since the 1990s has been the transition from the use of manually operated vibrating blades to lasers to cut corneal flaps.
Laser uses pulses to cut the flap for more uniform results, he said, cutting the risk of complications that resulted from too-thin or too-thick flaps, corneal abrasions or machines that jammed as they passed across the cornea, forcing doctors to halt the surgery.
While about 70 percent of Lasik surgery in the U.S. is performed with laser devices, Salz said, the less-expensive bladed tools are still in use. A laser costs $250,000 to $300,000, plus pricey service contracts, Salz said, compared with $40,000 or less for a manual blade.
While the use of blades to perform surgery can be perfectly safe, he said, he thinks surgeons should inform patients of alternatives – even if they don’t offer them.
“Particularly discount laser centers, they don’t go into this very much with patients,” Salz said. “They don’t say, ‘You know, there’s another way to do this.’ … Consumers have to be a little suspicious of discounted Lasik surgery. Why is one guy able to do it for $800 when everybody else charges $2,500? The reason is they’re usually not using a laser to make the flap.”
Lasik isn’t for everyone
Armed with better imaging technology and the tools to analyze the data they gather about their patients’ eyes, doctors are better now at identifying bad candidates for Lasik, Kontos said.
“The key is to screen out patients,” said Kontos, who said he turns down patients for Lasik every week, steering them toward other options.
The shape of a patient’s cornea, for example, might create a weakness that surgery would weaken further.
Improved technology has also allowed doctors to better customize treatment, he said.
Doctors used to base Lasik treatment – how, exactly, they’d reshape their patients’ corneas – on the patients’ prescriptions for glasses. Now their treatment is more customized, based on the digital images of their eyes, Kontos said.
When Kontos started performing Lasik surgery, about 20 percent of his patients had to undergo a second surgery for fine-tuning, he said. That’s down to 3 percent, he said.
He said he also hears fewer complaints about glare after surgery, which he credits to improvements in treatment.
Despite the advances, though, Lasik doesn’t necessarily last forever, and it doesn’t preclude later eye problems, such as cataracts.
“I have a handful of patients that over 20 years I’ve lasered three times,” Salz said. “Although most eyes are stable in the 20s and early 30s, not all eyes are stable. Some eyes change. They get more nearsighted, because the eye grows a little bit. Farsighted eyes are harder to correct and they tend to lose some of their effect, so it’s not uncommon to correct a farsighted patient when they’re 30 or 35 and have them need a touchup by the time they’re 40 or 45.”
And – perhaps most distressing for patients whose motivation is vanity – patients with Lasik-corrected vision might still need reading glasses, Kontos said.
“The aging eye can still lose the ability to see up-close,” he said. “Lasik doesn’t stop that.”