Scene of an anatomy: Lab offers students an inside look at human health
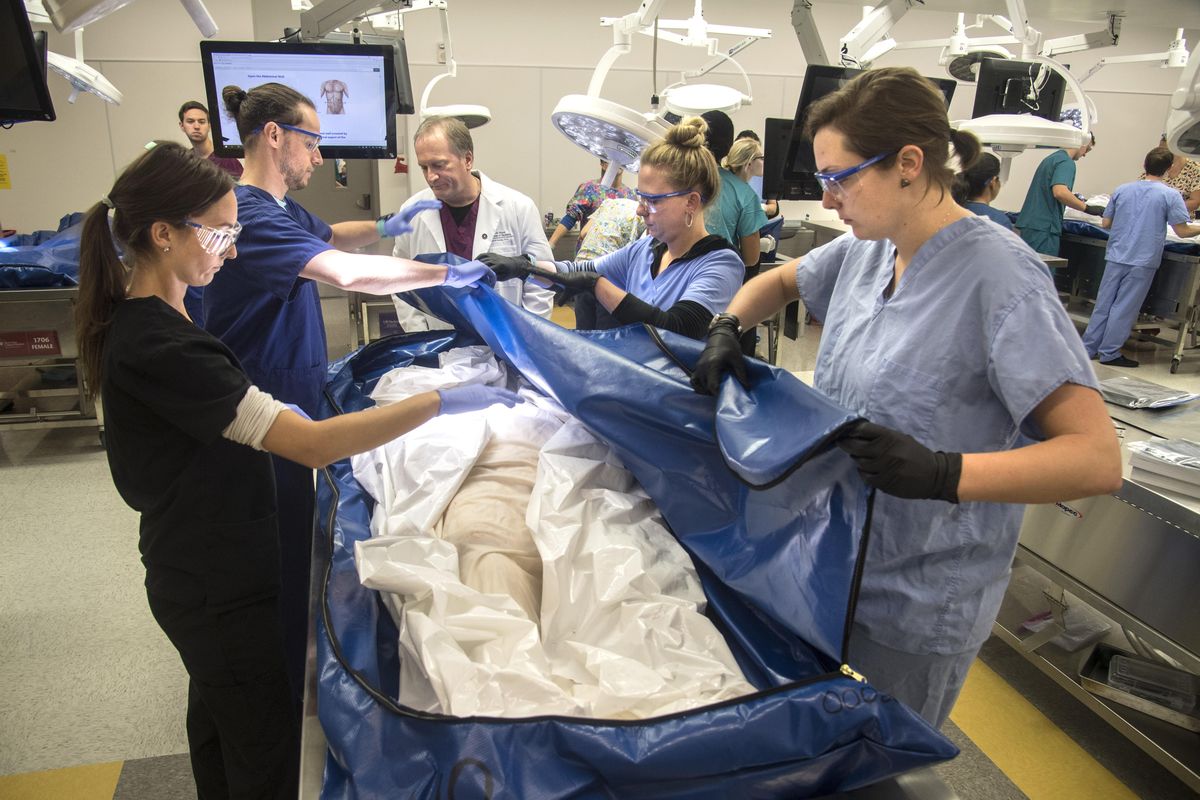
By the midpoint of a three-hour anatomy lab at Washington State University, one thing was clear: no two pancreases look alike.
Students at the Elson S. Floyd College of Medicine were in their third week of what may be, to outsiders, one of the strangest parts of medical school curriculum: dissecting cadavers.
Variations between dissection tables emerged as students worked within the abdominal cavity. Some abdomens contained healthy-looking pancreases; others showed swelling or signs of disease. Appendixes provided their own challenge. Some groups found the organ easily, while others had trouble or discovered their donors had had it removed.
When studying the human body from the inside, you never know what you’re going to find.
“I always call it the Forrest Gump lab,” said David Conley, professor of anatomy and director of the university’s Willed Body Program.
As the lab progressed, students called other groups over to their tables to see variations between healthy- and unhealthy-looking organs. Some sketched diagrams on the whiteboards lining the walls.
“It’s your first patient,” student Rebecca Gold said of the cadavers.
It’s an exercise the students, and the college, take seriously.
Privacy laws prohibit students from knowing the identity of their donors. They’ll never learn whether the body belonged to a fellow Coug or why that person might have wanted to donate.
That informational distance creates an odd sort of intimacy: Students hold organs in their hands, discuss their functions, peer not just at bodies but into them, all without ever knowing the bodies’ names.
The labeled dissection tables simply denote “male” or “female” with a four-digit identification number. Though students will examine the face and head later in the semester, both remain covered for now.
Still, the college knows it’s teaching more than anatomy.
“It’s the first experience with death and the deceased for some people,” Conley said.
Weeks before lab starts, students get a chance to meet the body they’ll be working with for the rest of the semester.
They take notes about tattoos, signs of disease and medical devices – everything visible that makes their donor unique. Then they write a reflection about what they suspect their donor’s life might have been like.
“It gives a lot of humanity to it,” said Kendal Dean, another student.
WSU’s Willed Body Program has operated since 1972, supplying cadavers to undergraduate anatomy classes and other health science programs. The school is one of three universities in Washington with such a program, alongside the University of Washington and Pacific Northwest University of Health Sciences in Yakima.
With the opening of WSU’s Spokane medical school, the program moved from the Pullman campus, and the need for donations has increased.
Many donors are loyal WSU alumni who want to help the college, Conley said.
“They see it as a way to make their body useful after death,” he said.
Others choose donation because it’s cost-effective. Donors may need to pay for transportation to WSU, depending on where they live, but the university takes care of all other costs.
Bodies are embalmed and cremated when work on them has been completed. Families can choose to have the cremated remains returned to them or opt for burial at Greenwood Cemetery in Palouse, Washington. There, a special plot is reserved for the university’s medical donors, with a plaque thanking them for their contribution to science.
Cadaver dissection has long been a part of medical school, taking off in England in the 17th century. In its early days, however, the practice was once conducted along considerably less savory lines.
By law, the bodies of people convicted of murder and other heinous crimes were made available for dissection. The sentence was considered worse than death because of the Christian belief that proper burial was essential for a successful transition to life after death.
The supply from the hanging of criminals failed to meet demand for the fast-growing field, however, and many anatomists either paid body snatchers or entered cemeteries themselves to steal the recently deceased. Not surprisingly, the general public thought rather poorly of the profession as a whole. Eventually, reforms to medical schools would do away with the practice.
With advances in technology, some medical schools have moved entirely away from cadaver dissection as a method of teaching anatomy, saying it takes valuable time in an increasingly crowded medical curriculum and is too costly.
Instead, they use prosections: dissections done by advanced students and anatomy professors to highlight specific systems within the body. Some also incorporate 3-D digital models.
Conley, however, is adamant that there’s no substitute for the full anatomy lab experience, because real human bodies rarely look like illustrations in textbooks.
“Even though they have these atlases that make it look like everybody’s built the same way, they’re not,” Conley said.
His students agree. Eric Stiles, a medical student, said one of the main reasons he wanted to study at WSU was the fact that they still do a full anatomy lab.
“You actually get to learn what the body looks like,” he said.
Stiles said his father was so moved watching his son’s white coat ceremony marking the start of medical school that he decided to will his body to the college’s program that day.
Over the course of the eight-week lab, students are preparing for a final presentation, where they’ll lay out how they suspect their donor died.
Some groups said likely causes of death were apparent after the first week, when some cadavers showed signs of heart disease and strain. Others formed theories during the abdomen lab after noticing diseased organs. Still others said nothing apparent had shown up.
The benefits of working directly with cadavers goes beyond learning anatomy. Students work in groups of four or five, so the lab provides one of their first experiences of teamwork in a medical setting. And the lab can help students realize whether a career in surgery is right for them.
Seeing multiple artery stents or signs of scarring on the liver reminds students of the health impacts of surgeries and chronic diseases. Student Katie Schmidt said it emphasized the importance of preventive medicine for her.
Others in her group said learning with a real body helped them better understand body systems, not just parts. If an organ they’re looking for isn’t apparent, students have to work to find it, using their knowledge of vein and ligament connections, or nearby organs, to arrive at a location.
“It makes us think critically,” said Patrick Miller.
Calling the donors “first patients” is more than a marketing line. Conley and other doctors say they vividly remember their first anatomy classes and often thought back on the sessions in their early years practicing medicine.
“It’s an experience (students) will probably remember for the rest of their life,” he said. “It’s a perpetual gift.”