Dr. Tim Chestnut brings personal experience to his work helping amputees
Dr. Tim Chestnut jokingly tells patients he’s the bulldog. He’ll fight for amputees if they need more advanced prosthetics for work or active lifestyles.
For several years, he has put medical teeth behind that offer, working with Spokane specialists in a program where he examines amputees and completes medical reports crucial for receiving devices.
Newer insurance rules require a physician to document an amputee’s medical condition and detailed prosthetic needs, so Chestnut, an internal medicine doctor, does so regularly. An amputee himself for the past 12 years, he also brings empathy to the exam room.
“I became aware of what amputees go through within the health care system; it’s embarrassing,” said Chestnut, who also teaches in Spokane for the University of Washington School of Medicine.
“Amputees are not treated well. There are strict documentation rules that have to be followed in order for patients to get prostheses, and if not, they’re often delayed or denied getting them.”
It was a 2002 accident at his home that led Chestnut on a path to understanding what amputees face. A barn he was working on collapsed from a strong wind gust and dry rot damage, and the roof beam crushed his right ankle.
Although Chestnut had surgery immediately after his injury, it had been a “really ugly fracture,” he said, and there were complications. His ankle never really healed, and then the bone died because of poor vascular circulation to the area. Bone grafting wasn’t an option.
“The only opportunity at that point was amputation, which was done in January 2006,” he said. “I got fantastic medical care, but if something could go wrong with my amputation, it did.”
Issues included a socket fitting and insurance complications, among other delays, and he wasn’t able to walk well for a year or more.
“I was frustrated,” Chestnut said. “Then I got talking to prosthetists and other amputees, and I learned there were a lot of amputees who were having more difficulties than me.”
He previously worked in Spokane as a pulmonary critical care physician, but now focuses mainly on teaching, consulting and working with amputees. As a clinical assistant professor, he teaches classes for first- and second-year UW medical students based on the Gonzaga University campus.
After a 2011 audit report, Medicare overhauled reimbursement, coding and clinical-care guidelines for lower-limb prosthetics. The Office of Inspector General had determined the agency was spending unnecessary millions on limbs for patients with other, more serious health problems, according to the Amputee Coalition, a national organization.
“The strict Medicare rules came about six years ago, and other insurance companies followed suit,” Chestnut said. “The result was many amputees were denied or delayed getting prosthetics, and prosthetists weren’t getting paid. About 20 to 25 percent of them went out of business.”
Prosthetists today make their recommendations, but under the newer requirements, a doctor’s report must detail the final prosthetic components needed and include a medical checklist, said Jim Cahill, co-owner of Thompson’s Custom Orthotics & Prosthetics in Spokane.
To help patients navigate the rules, Chestnut along with area prosthetists developed a program to meet requirements and shorten wait times, Cahill added.
“Medicare sort of changed the rules, so our (prosthetists’) documentation was no longer considered part of the medical record,” Cahill said. “We needed a medical doctor to dictate what parts are needed for the prosthesis.”
The rules for determining the type of prosthesis and its high-tech features are based around a patient’s activity level, he added. “It’s up to the physician to determine potential for that.”
“We had to ask physicians for documentation, and ask that they amend notes. It really slowed the process because we had to have additional documentation. Dr. Chestnut stepped in, and it’s a good team approach. We’ll see a patient. We’ll do our evaluation, and we refer them to Dr. Chestnut.”
The review could be for an initial prosthetic, a replacement or even supplies for the device.
Chestnut does two key steps, Cahill said, one being a required “head-to-toe” physical of the patient, which the doctor does in the prosthetist’s office. Then he writes up required medical reports incorporating specialists’ recommendations.
“Mostly, it speeds up the whole process for the patient,” Cahill said. “What should take two weeks now takes two weeks from beginning to end, when initially as Medicare started changing the rules, it was slowing things down to where everything was taking months.”
Chestnut credited the work in the past few years as a joint effort among amputees and prosthetists, with him evaluating patients for three Spokane-area practices.
“I went to every insurance company and downloaded the detailed requirements that have to be included in the reports; that prosthetists are required to have in their charts before amputees can get what they need,” Chestnut said. “Most primary care physicians aren’t trained to write those reports.
“We developed a program to where I’d go to the prosthetist’s office, I’d see patent, I’d do an evaluation, and then generate the report and make sure the report has all the information necessary for that particular insurance company and patient.
“It’s very collaborative. I’ll talk with the prosthetist.”
The program is working, he said, citing numbers.
“Within the past five years, we went from having 80 to 85 percent of advanced foot prosthetics denied to now less than 5 percent,” Chestnut said.
Younger patients tend to need support after an auto or motorcycle accident, or following an industrial workplace incident, according to Chestnut. Older amputees typically face the issue because of advancing medical problems such as from vascular disease or diabetes.
His advocacy work, including support for a patient if an insurance company denies a request, can be time-consuming. However, Chestnut said he’s seeing fewer contested cases.
“I have two ongoing cases right now for advanced prosthetics; we’re going through the appeal process. There were times in the past we had 20 appeals going on. We’d win the vast majority. Once they realized the program we developed, they quit turning as many down.”
He’s concerned that some places in the U.S. have around 75 percent denials for advanced prosthetics.
“They may get a prosthetic, but they get a basic prosthetic that doesn’t allow them to go over uneven ground, or carry a load in the shop, or golf,” he said.
Financial hardship for amputees is another concern, Chestnut said. He is working with other amputees to start the Prosthetic Assistance Foundation in Spokane to offer financial assistance for patients. The recently formed group will soon seek grants.
“Most amputees have complications, and it’s a financial hardship for them because prosthetics are very expensive,” Chestnut said. “The Affordable Care Act has made it more expensive because of the co-pay and deductible required.
“That’s a financial struggle I see every single week for my patients.”
Examples include a $2,000 deductible, which he said is common, and an additional $2,000 to $3,000 in required co-pay if it’s set at 20 percent of a basic foot-ankle prosthetic cost, typically at $10,000 to $15,000, he said.
“And it’s three times that amount if it’s above the knee,” Chestnut added. “It’s a huge problem that’s unanswered right now.”
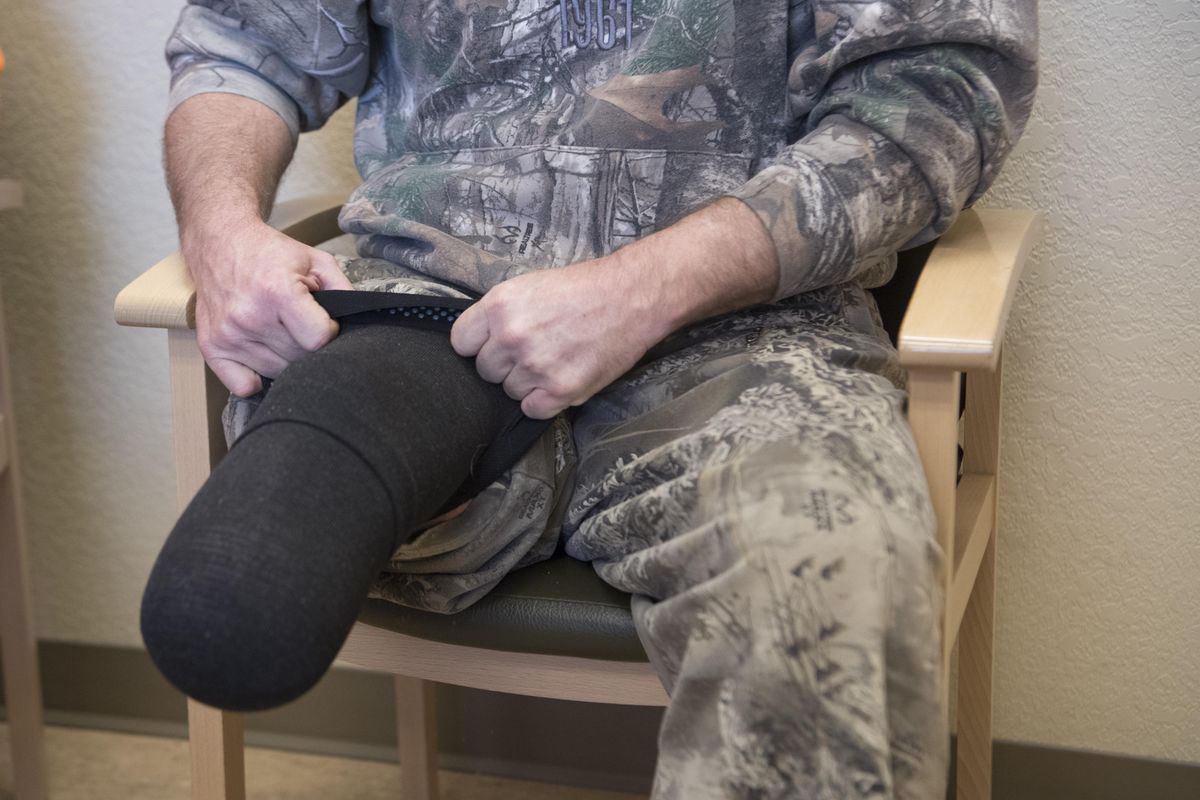
He shows his own prosthetic, pulling up a pant leg.
“This is a foot-ankle prosthetic with a socket; mine is more advanced at about $15,000 to $16,000 in today’s dollars. If you have a deductible and copay of 20 percent for this, what you come up with might be $4,000 to $5,000 out of pocket.”
It helps that Spokane-area amputees have someone like Chestnut in their corner, Cahill said.
“He just really has a good rapport with patients,” Cahill said. “He’ll stand up for them if need be.”
(509) 459-5439
treval@SPOKESMAN.com