On pins and needles: Millions choose acupuncture for relief
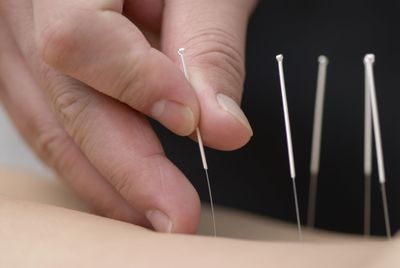
Kaiya Larson pressed a small, thin needle against the patient’s skin. A licensed acupuncture practitioner, Larson focused intently as she felt for the right spot, then – ping! – she pushed the needle in and twisted it a little to the right, as though she were turning up the volume on her car radio.
The 31-year-old patient, hoping that acupuncture would increase her energy level and relieve her occasional stomach problems, said she felt a brief “grab.” Then nothing.
She lay on the exam table for 20 minutes more while that needle, and four others, remained in place.
Larson, demonstrating the procedure at the Tai Sophia Institute outside suburban Columbia, Md., had already taken the patient’s pulses; in Chinese medicine, there are six of them, which measure not heartbeats but energy flow, and are taken at two levels of pressure on both wrists.
Besides having a discussion about the patient’s general health, she had also examined the woman’s tongue, finding diagnostic clues in its color and texture.
The process bore little resemblance to a visit to a conventional American doctor. But it’s becoming familiar to an increasing number of Americans.
A study published in December by the National Center for Complementary and Alternative Medicine, a part of the National Institutes of Health, found that 3.1 million adults and 150,000 children used acupuncture in 2007, seeking relief from ailments including headache or back pain, insomnia and attention-deficit disorders.
That was about 1 million more adults than in 2002, when the last NCCAM survey was done.
“In the consciousness of the American public, acupuncture has become white bread,” says Joseph Helms, a physician who trains medical doctors in acupuncture techniques.
The people who go regularly for treatment swear by it. Others scoff that it’s complete hokum.
The American Medical Association takes no specific position on acupuncture; the AMA groups it with other alternative treatments, saying “there is little evidence to confirm the safety or efficacy of most alternative therapies.”
In 2007, NCCAM spent about $9.1 million on acupuncture research. While more is planned, Brent Bauer, an internist at the Mayo Clinic and director of its complementary and alternative medicine program, says the research is in its “toddlerhood.”
“Some of the most interesting research on acupuncture is how it might impact brain functioning,” says Richard Nahin, acting director for research at NCCAM.
Magnetic resonance imaging observations during acupuncture have shown specific areas of the brain that respond to the treatment, he says. The field of pain relief is getting the most attention in these studies, but they hold promise in many areas.
Bauer also says he has seen remarkable results in pain management, adding, “I don’t fully understand how it works.”
In 2004, researchers at the Center for Integrative Medicine at the University of Maryland tested the effects of acupuncture on 570 people over 50 with osteoarthritis in the knee.
The patients were split into three groups: The group that received education about their condition recorded a 22 percent improvement in function; those who received sham acupuncture, a placebo-like process using real needles but not on known acupuncture points, improved 31 percent; and those who were treated with true acupuncture recorded improvement of 40 percent.
The benefits of the actual acupuncture showed up over time, with most of those who got relief feeling it after 14 weeks of treatment.
Other preliminary research shows promise when acupuncture is used as part of treatment for infertility, obesity, post-traumatic stress syndrome, depression and pain relief. But many of those studies were small, and more work needs to be done for them to be validated.
However, other studies have found no difference between sham acupuncture and the real thing. An analysis of 13 studies of pain treatment with acupuncture, published online this month by the journal BMJ, concluded there was little difference in the effect of real, sham and no acupuncture.
Bauer says that patients are increasingly asking about incorporating acupuncture into their care and that doctors, especially younger ones, are more willing to give it a chance.
“I would call it evolutionary,” he says of physicians’ attitudes. “Twenty years ago there was more antagonism and much more hard-core skepticism. Now there is a lot more of an open attitude.”
Brian Berman, director of the University of Maryland center, came to acupuncture after feeling that something was missing in his practice of family medicine.
“I was well trained with acute problems such as an asthma attack, trauma, heart attack,” he says. “But when it came to chronic pain, I didn’t have all the answers.
“Eventually that led me to taking the acupuncture course in 1983, then further training in the U.K., and I incorporated it my practice.”
When he first suggested it to his patients, Berman says, they were skeptical. They were looking for a “magic pill” that would cure them.
“Sometimes we had tried the pill and they still had their problems,” he says, “and I would ask, ‘Would you consider acupuncture?’ ”
Often, it worked.
Gastroenterologist Linda Lee, director of Johns Hopkins’s new Integrative Medicine and Digestive Center, says it’s hard to find scientific support for acupuncture, but she sees anecdotal evidence.
“From a research point of view, I understand the criticism,” she says. “But we physicians are in the healing business, and we have to go beyond the pharmacological solutions to understand the whole person. Acupuncturists start with the whole person.”
Elise Feingold, 51, a human geneticist from suburban Silver Spring, Md., began trying acupuncture seven years ago for chronic back and knee pain.
She says she reaped unexpected benefits: dramatic and rapid relief from hot flashes that had been waking her seven or eight times a night, as well as relief from 11 months of coccyx (tailbone) pain that her doctors had been unable to help.
“You see benefits over a period of time,” says Feingold. “You’re not always going to have that home run like (with) the hot flashes.”
She says she has also found relief for less tangible and perhaps more emotionally based issues such as sleeplessness and stress, some of which she attributes to the time the practitioner spends talking with her.
“There’s a therapy aspect to this, too,” says Feingold, who gets acupuncture about once a month for general health maintenance.
“I decided to leave my science brain aside,” she says. “I felt it had helped other people, and it might help me. I don’t know how it works, but it’s got 4,000 years of Chinese medicine behind it.”