‘It feels like a war zone’: Inside the Deaconess ICU as COVID-19 rages
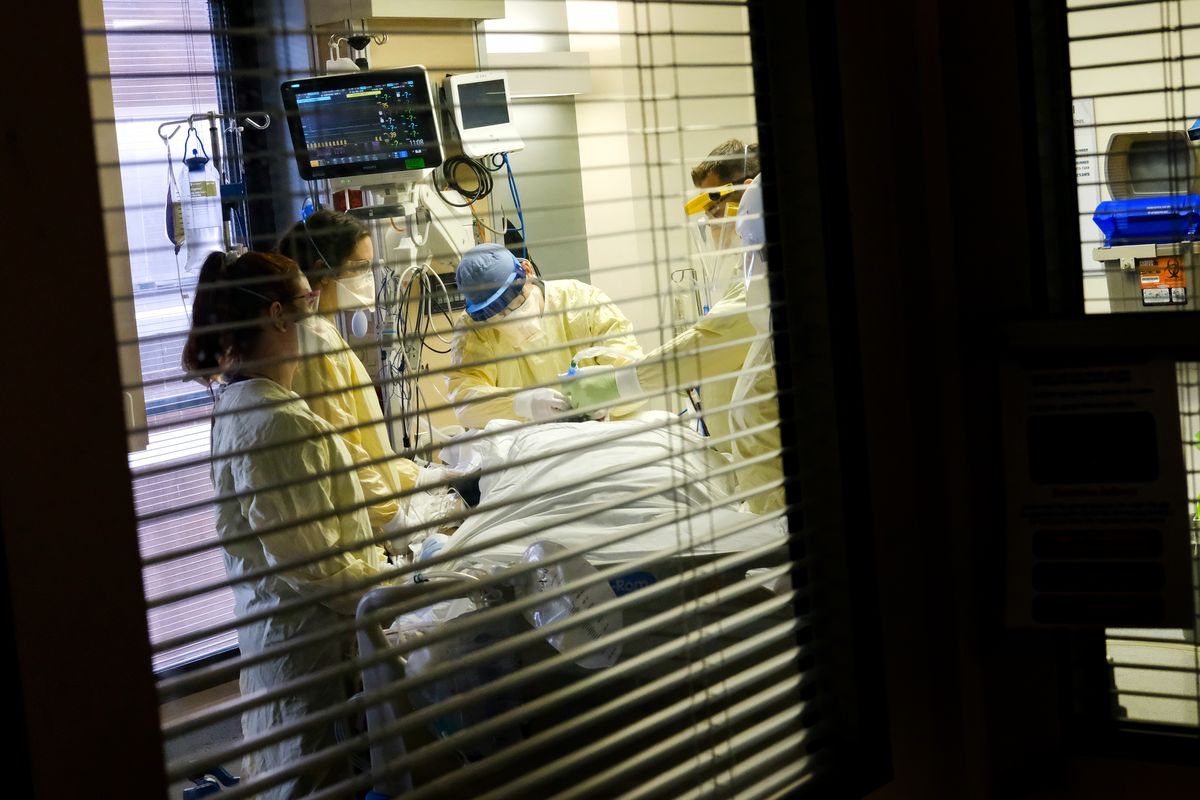
The COVID-19 ICU is quiet.
Ventilators hum inside patient rooms, and sensors beep. The phone rings occasionally: sometimes another hospital floor calling, other times a family member inquiring about their loved one.
Otherwise, there are no visitors, and only necessary staff roam the circular pod. Nurses stationed in front of one or a few rooms monitor their patients’ vital signs and huddle with doctors about treatment changes.
These patients are fighting for their lives. Caregivers are fighting burnout.
This is the intensive care unit at MultiCare Deaconess Hospital, where staff share the goal of defeating a virus that is ending lives and dashing morale.
“It’s ingrained in our brains that I can save that person; I am skilled enough to save that person,” charge nurse Kimberly Davisson said. “But with this pandemic, it’s like a losing battle every day. I can’t save that patient anymore because I am doing everything I can, but there’s nothing to fix them.”
Dr. Ben Arthurs, a critical care physician, was making rounds Friday morning at the hospital’s ICU, learning how patients did overnight. In many cases, he discovered they had gotten worse.

Because of the current COVID surge, hospital officials split the ICU into two floors, with the second floor for COVID patients and the third for other patients needing intensive care.
Seven of the nine COVID patients in the Deaconess ICU were on ventilators, sedated and lying still on their stomachs or backs, while the machine breathed for them.
Some of them might not wake up.
On Friday, half of the 18 occupied ICU beds at Deaconess were being used by COVID patients.
Patients are alone as providers can look in from behind the sliding glass doors that seal off the negative pressure air flow rooms, which resemble fishbowls. These rooms are outfitted so that contaminated air is sucked out of the room, keeping the air circulating and environment safer for health care workers.
IV drips and monitors attached to tall rolling stands are located outside each room, with long tubes stretching from the stand through a slit in the door, extending across the room to the patient.
Arthurs got the rundown on one patient from a team of nurses, a resident physician and other care providers. His takeaway is discouraging: The patient’s heart is starting to give out, so he talked with the care team about potential tweaks in medication.
Something more urgent was needed .
“If we’re going to give this guy any shot, we need to prone him,” he said.
A proned patient is one who has been positioned on their stomach. Proning patients, while not common at the start of the pandemic, is now happening multiple times a day in the ICU to help COVID patients breathe more easily, using gravity to help open up the lungs .

Davisson, the charge nurse that day, began gathering a team. Her role is to ensure that the ICU nurses have the support they need to care for patients.
On Friday, Davisson assembled a six-person team, including a respiratory therapist who leads the whole exercise at the head of the bed, with a mobility technician at the foot. Four nurses, two on each side, will move the patient up and over in the bed and flip them onto their stomach.
Another nurse stood watch outside the glass doors, ready to run for supplies if necessary, and checking the patient’s vitals.
One nurse at the foot of the bed is from the hospital’s cardiac unit, but as an “extender” nurse today, she’s helping when needed.
The team members all wore yellow gowns, gloves, N95 respirators and some variety of face shield. After removing all of the sensors from the patient, tucking the sheet around their body, they were prepared to move.
The respiratory therapist gave the team instructions and counted them down to each movement. It was choreographed and practiced. Some nurses watched for specific lines, like the dialysis, IV and ventilator tube, to ensure that none of those snagged with the repositioning.
After moving the patient up and to the side of the bed, they flipped the person onto their stomach.
No sensors went off, and the patient remained stable.
They would remain facedown for 16 hours.
‘I can’t do it anymore’
Staffing remains the hospital’s No. 1 challenge, and Davisson said sometimes that means cobbling a team together to flip a patient over or cover another person’s patient.
The problem is statewide.
On Sept. 3, the Department of Health requested 1,210 medical and support personnel from the federal General Services Administration, in response to requests from hospitals statewide. Since then, even more requests have been made.
The state has identified 10 hospitals where these staff will go, and as of Friday, the department is working on a process by which facilities will access these additional staff members.
In the meantime, hospitals are stretching their staff.
Typically, an ICU patient who might have acute kidney injury or failure will be on dialysis and get their own nurse. Otherwise, an ICU nurse would care for two patients at a time.
On Friday, one nurse was caring for three patients. Davisson is trying to give these nurses support in the form of an on-call “extender” staff member, who can run to get supplies, administer medicine or help flip a patient over.
Nurses from other parts of the hospital have joined the ICU for shifts lately, Davisson said, and burnout continues to be a real struggle.
“I went to a rapid response on the COVID floor, and the nurse was really struggling with what was happening with her patient, and she said, ‘This is my last week, I can’t do it anymore,’ ” Davisson recalled.
‘Like nothing I have seen’
Nurses are seeing younger patients in their ICU with the delta variant, including people in their 30s and 40s who are intubated, and these patients are staying longer in the hospital.
The longest COVID stays in the ICU have been five to six weeks, said Bryan Garrett, Deaconess ICU director, because these patients typically are healthier and have more reserve to fight the virus.
That doesn’t mean all of them will recover, though. When a patient first arrives in the hospital, they are likely put on high-flow oxygen, administered through either a mask that covers their nose and mouth or just their nose, in the hospital’s non-ICU COVID ward.
The COVID ward at Deaconess had 39 patients being treated on Friday. In total, Deaconess providers were treating 48 COVID patients that day.
MultiCare Valley Hospital had 29 COVID patients on Friday. There are more at Providence Health Care’s Sacred Heart and Holy Family hospitals.
The COVID ICU at Deaconess receives patients from the hospital’s COVID ward, the emergency department and, on occasion, transfers from outlying hospitals, when they have space.
“As they stay longer and longer and longer, their oxygen demands go up, and they’re so tired that they can’t do it anymore,” Davisson said.
That’s when they either ask for help breathing with a ventilator or a physician recommends it.
“We have patients that initially decided they didn’t want a ventilator and a week into their stay have asked for it,” Davisson said. “We’re seeing this a lot more now, especially with the younger demographics.”
Lee Rowe, an ICU nurse in the COVID unit, said patients who are considering going on ventilators are almost always afraid.
Social workers arrange video calls for patients before they get intubated and sometimes sedated.
It could be, for some patients, the last time they can say goodbye to family members.
“If we sedate them, that might be the last little glimmers of interaction with the outside world they’ll have, and I think some of them understand that,” Rowe said.
As a respiratory virus that attacks the lungs, COVID-19 makes it incredibly challenging for patients to breathe.
“This COVID virus is trashing people’s lungs, and it doesn’t matter how old you are,” Davisson said. “It’s like nothing that I have seen before.”
Younger patients are also requiring more lifesaving support the longer they stay in the hospital. If a patient’s kidneys fail, they are put on continuous dialysis.
But there are only so many lifesaving options.
If these patients survive, their long-term recovery and permanent medical outlook is bleak. When patients lose kidney function, for example, that could mean weekly dialysis appointments for the rest of their lives.
A ‘constant battle’ for hope
Todd Stewart has seen a lot as a 20-year emergency room nurse who shifted to the ICU seven years ago.
The rewarding part of his job always came from using his skills and training to make positive changes for his patients. COVID-19 has made that far more difficult.
“It’s this constant battle to not start to feel the hopelessness, because you have to be hopeful in order to give good care, right? But by the time you’ve seen your 100th one …” he said, looking at his patient who was completely still except for the ventilator pushing their chest up and down.
Stewart said he has not had a COVID patient older than 65 with diabetes survive so far, and treating younger COVID patients is no easier. That’s, in part, because typically being an ICU nurse comes with the potential for patients to get better. With COVID patients, it’s much less common to see that incremental improvement.
“We have plenty of ICU patients that get a tiny bit better every day and that sort of fosters this hope,” Stewart said. “But a lot of these (COVID patients), you can barely even turn them in bed without their blood pressure crashing.”
Those scenarios are demoralizing.
Arthurs does ICU shifts every few weeks. He said morale is down from even five weeks ago in the COVID unit, and his biggest fear going forward is that staff won’t have enough stamina to push through the surge of patients.
“Everyone is holding it together right now, but October and November worry me because of the risk of that really starting to take its toll on our staff,” he said.
Tough conversations
One of the most challenging parts of Arthurs’ week was spending two, three and four hours of each day on the phone with families whose loved ones are dying of COVID-19.
COVID patients are not allowed to have visitors, which has affected how care conversations go with family members.
Typically, when a patient is not doing well, and providers decide to talk to the family about the potential to take a person off life support, the family can come in and see their loved one.
Seeing a patient in person and understanding their pain is a part of what typically eases those decisions about end-of-life care, Arthurs said, and while providers can use video calling, it’s not the same.
While some older patients might have end-of-life directives, younger patients likely do not, which means getting the family’s direction is a part of the patient’s care.
Arthurs said it’s been draining to have these conversations over and over with families. There were eight such conversations scheduled on Friday alone for ICU patients, where physicians will ask families how they want to proceed with care, and, in some cases, recommend comfort care, taking the patient off the ventilator and saying goodbye.
“You’re trying to find a way to explain it in a way that families understand and not sound like you’re being pessimistic or hopeless and not leave them with the impression that you’re trying to take away things or ration care,” Arthurs said.
But the reality, as some nurses shared, is that many of these COVID patients on ventilators simply do not improve, even after weeks of treatment and a machine breathing for them.
It’s not just grief that providers have to process with families over the phone.
Arthurs and other providers are also fighting misinformation, or “Dr. Google,” and the supposed miracle cures for the virus that families find online and demand for their loved ones.
The most popular request is ivermectin, a drug used primarily in animals and that the Food and Drug Administration has specifically not authorized to treat the virus. Arthurs said he has to explain that while there might be plausible explanations at the petri dish level, there’s not enough clinical data to support its use.
“We’ve had to tell families ‘no’ and then we, in many cases, deal with a lot of initial reactive behavior and argumentativeness,” Arthurs said.
After hearing the families out and walking them through his own recommendations about what is happening with their loved one, they eventually see eye-to-eye.
“If I told my plumber how to plumb my sink based on what I saw on YouTube, and he told me that was against code, then I wouldn’t fight with him about that,” Arthurs said. “So I get pretty frustrated when people try to come fight with me about treatments.”
Worries in the ‘war zone’
Washington hospitals have not yet had to resort to rationing treatment or expanding care into nontraditional setting. But Idaho hospitals have had to move to these crisis of care standards. And with vaccine rates lagging in Eastern Washington, epidemiologists and physicians alike are very concerned for what the coming months hold.
At the Deaconess ICU, staff prepare for surges following big events.
“We try to preplan for seven to 10 days after a large event when people come up sick,” said Bailee Walters, the Deaconess ICU nurse manager.
So lately, things like the Spokane County Interstate Fair and big concerts at the Gorge Amphitheatre are on Walters’ and her team’s radar.
And while there were only nine COVID patients in the ICU on Friday, the team at Deaconess is actively preparing to expand its capacity.
The hospital has 30 ICU beds, but should they need to expand the COVID ICU capacity, they will move non-COVID ICU patients to the cardiac short-stay unit, and use the third floor for COVID patients as well, since it has negative air flow rooms.
ICU staff and nurses at Deaconess Hospital pleaded with community members to get vaccinated.
“The biggest thing we’re seeing is a lot of our patients are not vaccinated or half-vaccinated, and I think that says something about the severity of how people are getting sick,” Davisson said.
While vaccines are not 100% effective, “it sure saves you from going on a ventilator,” she added.
Just 52.4% of Spokane County’s total population has received at least one dose of a vaccine, according to the Department of Health, and 46.5% of all Spokane County residents are fully vaccinated.
This number is far too low for the community to achieve adequate vaccine coverage or herd immunity from the delta variant, said Eric Lofgren, epidemiologist and professor at Washington State University .
Estimates for herd immunity against the delta variant hover around 85% or higher, Lofgren said, meaning children who are not currently eligible will have to be vaccinated before communities can meet those thresholds. Public health officials expect vaccines for 5- to 12-year-olds to be approved for emergency use later this fall.
Even then, parents have to want to get their kids vaccinated.
Young people have the lowest vaccination rates in the state so far, which does not bode well for the fall and winter. Just 40% of 12- to 17-year-olds in Spokane County have received at least one dose of a vaccine.
Herd immunity will be difficult to achieve on a national and global scale for a long time, with vaccines not even accessible yet in some countries.
Lofgren and other epidemiologists are uneasy about the current situation in which the United States finds itself. Vaccine coverage is not adequate to stop the delta surge, and every unvaccinated person presents an opportunity for the virus to mutate into something worse.
“The more chances you get to roll the dice, the more chances you get to have something rare come up,” Lofgren said.
The worst-case scenario would be a new variant that can evade vaccines entirely, easily making targets out of all the fully vaccinated people.
The solution continues to be vaccines for everyone who is eligible, Lofgren said. With more people vaccinated, there will be fewer hosts for the delta variant, and with fewer hosts for the delta variant, the virus has fewer opportunities to mutate into an even worse variant.
“We’re still in a place where more people vaccinated is better,” Lofgren said. “And that’s important because every person that’s vaccinated is less likely to be hit by very severe disease, end up in the ICU and transmit it to other people.”
Statewide, there are 1,649 people hospitalized with the virus, including 274 patients on ventilators as of Sept. 16. With fewer people adhering to mask guidelines and no lockdowns in place, the potential for a worse flu and respiratory virus season is concerning to physicians and hospital leaders, since capacity is already so tight.
The stretched health care system continues to be the front lines of the battle with the virus, even if the world outside hospital walls has restaurants open, concerts happening and life appearing more normal..
“It feels like a war zone in here, and it feels like we’re doing mass casualty triage,” Arthurs said.
The hospital specialist who administers dialysis is having to make decisions about which patients to prioritize for the treatment.
While he’s not at the crisis point of having to take dialysis away from someone, that potential makes the coming months more foreboding.
“My biggest worry is that … the challenge, hopefully, will not be too much. But I think it’s going to be a huge strain,” Arthurs said.