Difference Makers: As COVID persists, so do the Inland Northwest’s health care workers
For the past nine months, nurses, doctors, respiratory therapists and critical care managers across the Inland Northwest have been fighting a disease they still know very little about.
The coronavirus pandemic has forced most people into their homes, but health workers continue to report to work.
They don uncomfortable, hot personal protective equipment. They manage entire COVID units in their hospitals. They become their patients’ caretakers and families as the quick spread of the virus means no visitors. They hold their hands, FaceTime their significant others or children and help those closest to them make the hardest decision they’ve likely ever had to face: when to administer end-of-life care.
When their shift is over, they go back home to their own families and communities, some of which still don’t believe the virus is real.
They’re exhausted, but the virus shows no signs of slowing. And neither do they.
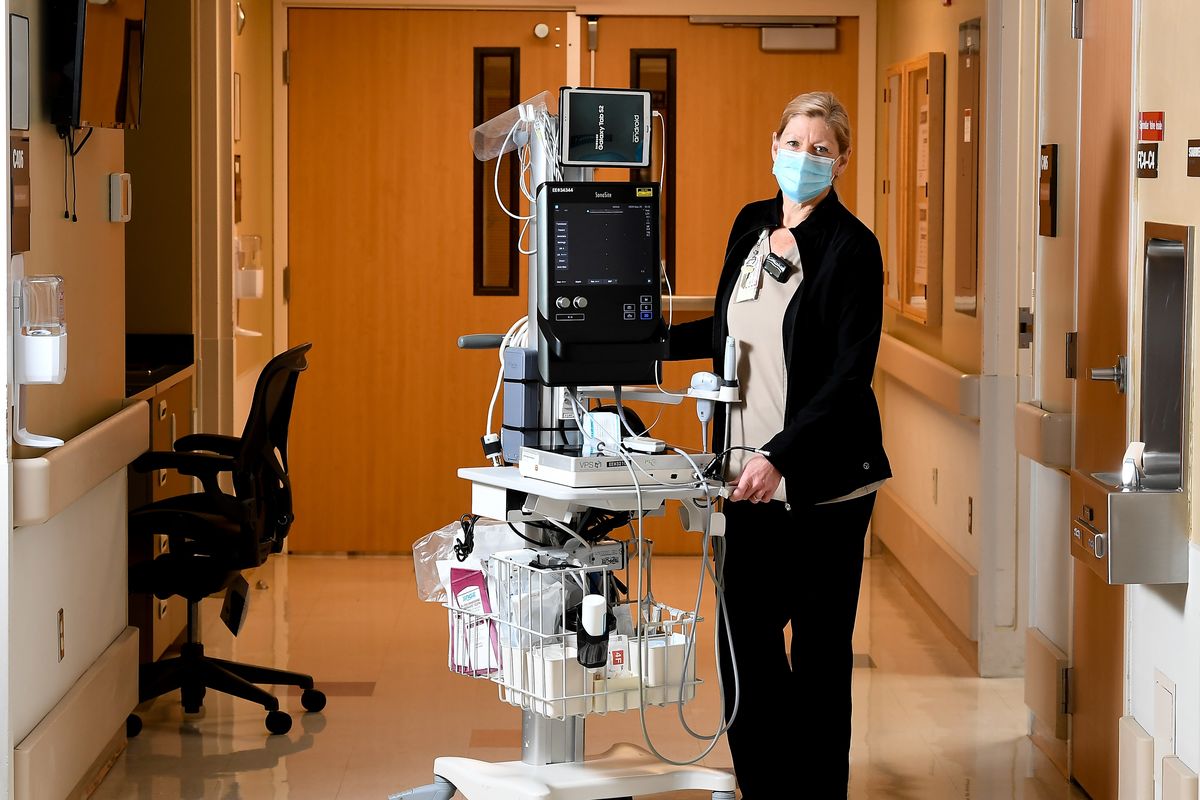
Terry Fisher, vascular access nurse at Mann-Grandstaff VA Medical Center
Every day at the beginning of her shift, Terry Fisher begins the process of donning her PPE. She fastens her gown, ties her mask, covers her face with a shield and puts on her gloves.
It’s hot, and it’s difficult to see and hear. But perhaps what’s even worse is how difficult it is to connect with her patients, who now only see her behind all of the equipment.
Fisher, 60, has been working at the Mann-Grandstaff Veterans Affairs Medical Center since 1990 after serving in the Air Force, but she’s never experienced anything quite like the COVID-19 pandemic.

“These people are scared, alone and extremely sick,” she said.
As a vascular access nurse, she works all over the hospital, performing central lines and starting IVs. She’s even been deployed to other VA hospitals across the country.
On a busy night shift in Montana, she checked on a patient who was critically ill and confused. He grabbed Fisher’s hands and held as tight as he could. He placed her hands under his chin and began to pray.
Fisher sat with him and listened. She was the only person there who could comfort him. When he was done, she released his hands, rubbed his head and left to check on other patients.
He was eventually transferred and later died.
It’s difficult for Fisher when people say the coronavirus is a hoax, that they don’t know anyone who’s died. She faces the reality of the virus every day and sees how quickly it can spread.
“They should count themselves as lucky,” she said. “Just because it’s not happening to you doesn’t mean it’s not real.”
Michele Goode, critical care nurse at Kootenai Health
When it’s time to withdraw care for a COVID-19 patient who is dying, Michele Goode allows two family members to come to the hospital and say goodbye.
Sometimes, the family wants Goode there. Other times, they don’t. And sometimes, family members can’t handle being in the room, so it’s Goode’s job to step in.
For the past nine months, Goode has experienced this over and over. She’s spent weeks as one of very few human contacts with the patient. She’s held up a phone to help video chat with loved ones. She’s talked through her patients’ situations with family members to help them choose when to issue end-of-life care, a decision that must be made over the phone.
Goode, who’s been a nurse for 12 years, is normally able to keep work at work, but the severity of this disease isn’t something she can leave at the hospital.
“It affects all of my everyday life,” she said. “It’s not something I can get away from.”

Goode, 45, has lived in Coeur d’Alene since 2003, and she knows many patients personally. She cares for her community, even if it doesn’t always understand the severity of the virus.
When community members argue about masking and social distancing or sometimes dispute the facts of the virus altogether, all Goode can do is continue to show up to work.
“For me, it’s 100%, absolutely a reality,” she said. “And not everybody sees that.”
Todd Putren, director of emergency services at MultiCare Valley Hospital
The biggest challenge for Todd Putren and his staff has been being unable to connect with patients. Wearing multiple layers of PPE means patients can’t really see their doctors’ and nurses’ faces.
Health care workers try to smile through their eyes, Putren said, but it’s not the same. So, he and a manager decided to print buttons for everyone on staff with their pictures. Some choose a funny picture; others, a serious one. Putren’s is a photo of him and his wife – “because that’s who I am.” He wears it at all times.
“This way, the patient can see your face and connect,” he said.

The buttons are one example of how Putren, 45, and his team have come up with creative solutions to serve their patients during this unprecedented time. He’s been a nurse for 21 years, mostly in a leadership role, but as the director of emergency services, leading during a pandemic is completely different than any other experience.
Putren said he’s been impressed with how his team has been able to come together, as they have to constantly adapt to new practices.
Every single member of his staff has had their own personal challenges during the pandemic, Putren said, but they always put their patients first. It might be especially true for himself, as COVID has become increasingly personal for him. Both of his parents contracted the virus. His father, who had other health conditions, died.
It’s made the severity of the disease all the more real to him.
“There’s been moments when I’m in tears,” he said. “You never imagine. It was so unexpected.”
Erica Mazzarella, respiratory therapist at Kootenai Health
At first, it didn’t seem like Idaho would be hit that badly. But slowly throughout the summer, Erica Mazzarella watched as the numbers continued to go up.
Now, the emergency room sees one COVID patient right after the other, and it seems like the hospital is getting closer to Mazzarella’s worst fear: not having enough equipment or staff to care for everyone who comes in.

Mazzarella, 49, works with COVID-19 patients every day and helps administer and manage breathing treatments, whether it be a ventilator, a BiPAP machine or a high-flow oxygen machine.
Lately, she’s worked with her staff to prone her patients, meaning they turn them a certain way to improve oxygen flow.
“With COVID, it takes forever for people to get better,” she said. “Sometimes we’re not able to help them. It’s heartbreaking.”
It’s difficult for Mazzarella when her community doesn’t accept the reality of the situation. She’s seen husbands and wives sick together but forced to be in separate rooms. She’s talked with patients when they feel scared and alone. She’s had discussions about who should receive which respiratory equipment because the hospital is so low on supplies.
Still, people don’t understand that wearing a mask is important, she said. They don’t understand that the hospital can only take care of so many patients, and beds are filling up.
“It is real,” she said. “It’s not a myth. It’s not political. Once it hits, it spreads.”
Bailee Walters, critical care manager at MultiCare Deaconess Hospital
Bailee Walters was in a meeting with other hospital staff one morning when she got good news: one of the ICU’s first COVID patients was finally going home.
It was early on in the pandemic, and the patient had been in the hospital for weeks, amid so many unknowns surrounding the virus. Hearing that they finally got to go home, Walters said, was overwhelming.
As a critical care manager at MultiCare Deaconess Hospital, Walters, 32, is a facilitator. She ensures nurses have the skills and supplies they need. She partners with other hospital departments to provide the best care for those in the ICU.
In the spring, her job became consumed by COVID-19, as the hospital decided to open a ward to keep patients sick with COVID separate from the rest of the hospital. She helped coordinate the move and the hospital’s surge plans, in case it became overrun with patients.

“That was the moment I realized this wasn’t your typical bug,” said Walters, who has been at Deaconess for almost two years.
Her son calls health care heroes – “because they save people” – and when she watches nurses do their job, she knows it’s true.
Walters got into this career to help patients so they can leave the hospital and live their lives. Hearing one of their very first COVID patients could go home was so rewarding, she said. It meant she and her staff had succeeded.
We did it, Walters remembered thinking.
We can conquer this.