Can total joint replacement restore your quality of life?
If you suffer from joint pain, you know how it can greatly affect the quality of your life. The chronic aches, swelling or sharp pains in the hip or knee can keep you up at night, limit movement and diminish your ability to do the things you love.
Joint problems are more common in older adults, but that doesn’t mean younger adults aren’t affected, too. Sometimes joint pain is the result of a sports injury or accident, or it can be attributed to osteoarthritis, also known as “wear and tear” arthritis.
“The most telling sign of osteoarthritis of the hip or knee is a chronic dull, achy and deep pain in the groin or knee that occurs with walking,” said Joshua Drumm, D.O., a fellowship-trained joint replacement surgeon at Providence Orthopedics & Sports Medicine in North Spokane. “The pain generally gets better with rest and/or with anti-inflammatory medications. It typically hurts at night, frequently waking people from sleep.”
When to consider surgery
There is a broad range of non-surgical treatments that can help provide pain relief and maintain your mobility. Physical therapy, bracing, cortisone injections and anti-inflammatory or pain medications are a few examples of treatments that can help mitigate the pain or discomfort.
However, if hip or knee pain continues to affect your ability to walk, work, sleep or even sit for longer than a few minutes, then consider getting an evaluation for a surgical procedure, such as total joint replacement.
While there are different types of joint surgeries, depending on the joint affected and the symptoms, total joint replacement is one of the most common surgeries for people experiencing chronic joint pain in the shoulder, hip and knees.
What is a total joint replacement?
“Joint replacement is a term we use to help simplify the idea of what we are doing. In reality, especially in the knee, it is more of a resurfacing,” said Dr. Drumm.
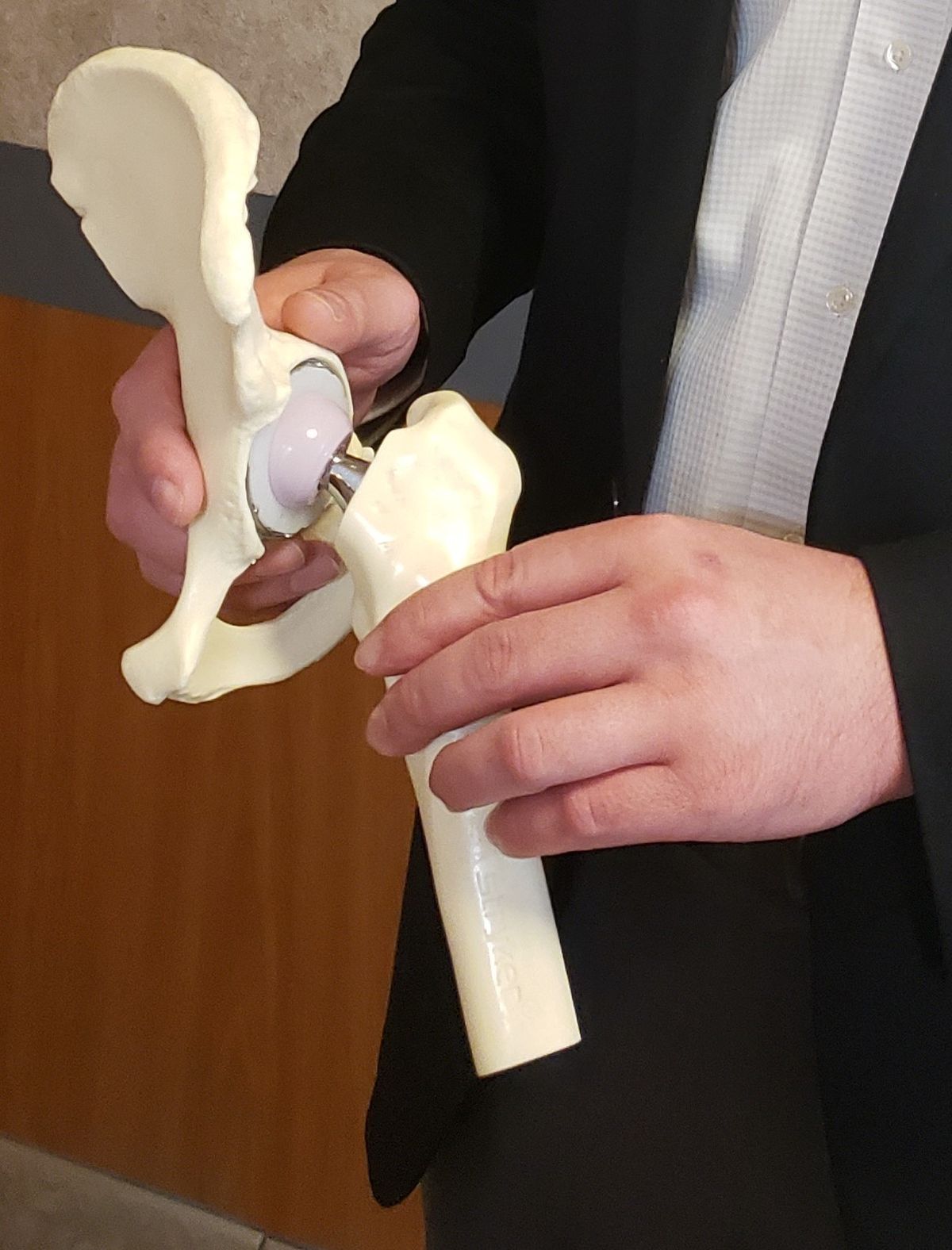
“For knee replacement, we are simply removing the diseased cartilage from the femur, tibia and patella. Then we resurface the bone with metal and plastic. For the hip, we remove the cartilage from the socket and resurface it with metal and plastic. The femur has a stem placed in the canal with a metal or ceramic head. So, to be clear, the surgery for the hip is more of a replacement.”
Dr. Drumm explained there isn’t an average age for patients who choose total joint replacement. “You’re never too old or too young. Joint replacement is a quality-of-life procedure. If you have bone-on-bone osteoarthritis of the hip or knee you’re a potential candidate.”
How to prepare for total joint replacement surgery
If you think total joint replacement might be an option, there are a number of things you can do to set yourself up for the best possible outcome.
The Total Joint Program at Providence Orthopedics & Sports Medicine prepares patients for the entire journey: before, during and after joint replacement surgery.
“From the moment a patient is referred to one of our orthopedic specialists by their primary care provider, the entire care team here encourages them as well as their support person to participate in our education program,” said Laura Waters, RN, Total Joint Program manager at Providence.
The education program begins 4-6 weeks prior to your procedure and includes interactive online Zoom courses where you can ask questions and hear the answers to other patients’ questions. There’s also a PDF version of the course that can be emailed or printed, as well as a recorded version for patients who prefer to watch a video.
“We encourage caregivers or primary support persons to also attend the classes because we offer information about how to prepare the home for post-surgery, and what to expect during the patient’s recovery,” said Waters.
Another way the Providence team prepares you for joint surgery is by assessing your need for certain exercises or strength training before the procedure. You also undergo a risk assessment to ensure you’re in the best health possible to go through an elective procedure.
“If a patient isn’t in optimal health prior to surgery, we might refer them to another specialist to get them as prepared as possible for the best outcome,” said Waters.
Outpatient surgery is an option
In the past year, the COVID-19 pandemic created an opportunity for the Providence orthopedics team to further enhance their outpatient joint surgery procedures while following all Centers for Disease Control and Prevention (CDC) guidelines for COVID-19. Outpatient surgery means a patient leaves the hospital the same day as surgery.
“We’ve developed different care pathway options for our patients, based on their needs but with the goal of getting them home as quickly and as safely as possible,” said Waters.
While some patients choose to have outpatient surgery, other patients might require or want a short stay, where they can remain in the hospital and go home in the morning. The decision to have outpatient surgery versus staying overnight is a shared decision between you and your surgical team.
Recovering from total joint replacement surgery
Just as preparing for total joint replacement varies depending on your situation, type of surgery and health, the recovery process and recovery time vary, as well as how you experience pain.
“Knee replacement surgery hurts,” said Dr. Drumm. “In my practice we have you walking the day of surgery, and most of my patients go home the day of or the morning after surgery. The first week or so is quite painful, but we give you medications to help with that.”
The Providence team recommends you start physical therapy within two or three days of surgery. Most patients go to their physical therapy appointments, but if a patient needs in-home appointments, Waters said they’ll set those up in advance.
Hip replacement tends to be much less painful with a more rapid recovery. “Most of my patients go home the day of or the morning after surgery. However, pain is much less of an issue than it is with knees,” said Dr. Drumm. “With hip replacement patients, we typically have to convince them that they have not healed as much as they think they have.”
Regardless of the joint replacement procedure you have, the first couple days following surgery are about total recovery. You’re encouraged to “take it easy” but also to try to move around as much as you can tolerate.
Setting our patients up for success
One of the latest developments in orthopedic surgery with regard to joint replacement surgery has been the development of the Enhanced Recovery After Surgery (ERAS) program. “This allows us to optimize patients prior to surgery for better success afterward,” said Dr. Drumm.
This approach has been well-received by patients.
“The best feedback we’ve got is how well-prepared patients are before their surgery,” said Waters. “This greatly decreases their anxiety all along their journey and increases their positivity because they’re able to play an active role in their health care. We’ve also got great feedback from the care team. They can tell when a patient has gone through our courses.”
If you’re experiencing joint pain and want to know more about total joint replacement surgery at Providence Orthopedics & Sports Medicine:
* Register here for access to our free joint pain webinar series.
* Request a consult to meet our expert care team by calling (509) 252-1977.
Providence Orthopedics & Sports Medicine offers both surgical and non-surgical options for treating pediatric and adult orthopedic needs. Whether it is caring for your bones, joints, ligaments, tendons, muscles or nerves, the team of surgeons, doctors, physician assistants, nurses and rehabilitation specialists provide superior care in joint replacement, musculoskeletal oncology and trauma, fracture care, and sports medicine. As the region’s leading orthopedic practices, the program is recognized with multiple national awards and distinctions for demonstrating expertise in treatments, affordable cost, and better overall patient results. Our board-certified and fellowship-trained providers offer care in all sub-specialty areas, illustrating a commitment to personalized, quality care.